Podiatry
Podiatry  is a field of medicine and cosmetology that deals with the treatment and care of skin problems within the feet. Among the podologic treatments, essentially, the patients with limited mobility, skin diseases, bones and joints, metabolic diseases (diabetes), patients with faulty foot and finger deformities (bunions, toes), with foot problems, i.e.: imprints , calluses, warts, as well as ingrown or fungal nails, sweating feet, cracks on your heels should embrace it.
is a field of medicine and cosmetology that deals with the treatment and care of skin problems within the feet. Among the podologic treatments, essentially, the patients with limited mobility, skin diseases, bones and joints, metabolic diseases (diabetes), patients with faulty foot and finger deformities (bunions, toes), with foot problems, i.e.: imprints , calluses, warts, as well as ingrown or fungal nails, sweating feet, cracks on your heels should embrace it.
Clinical problems, relating to feet, can be treated in a podiatric office:
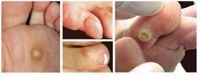 IMPRINT
IMPRINT
Symptoms:
- hard growth on the skin of the toes,
- pain with direct pressure on corn
- it may develop inflammation accompanied by pruritus and erythema,
- discomfort while walking in footwear,
- is more common with women
The most common location: around the heel, arch of the foot and the plantar side of the fingers.
Causes:
- wearing incorrectly selected footwear (too tight or too loose)
- bone defects of the feet (eg. bunions, bunionettes)
- stitching or bond inside the shoe, wiping fingers
- Long-lasting inclination of the foot (eg wearing high-heels)
Prevention:
- wearing correctly selected footwear (length, width)
- avoidance of wearing tight socks / tights
- in the case of the presence of epidermal thickening, use of special exfoliating cosmetics
- use of orthopedic insoles in cases of bone deformation / defects of the feet
In the podiatric office: removal with the use of cutters to remove the core; if necessary, the treatments are repeated cyclically.
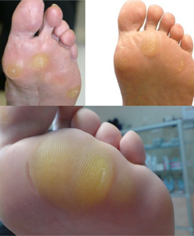 POROMA
POROMA
Poroma (calla, callus, tyloma) – limited thickening of the stratum corneum caused by repetitive pressure. Poromas are blurred from the healthy skin and have a yellowish hue. In the event of their rupture, pain may occur due to the accumulation of multiple layers. In contrast to corn, their central part does not have a horn.
Symptoms:
- tough, yellowish growth without a central horny pivot,
- pain or burning, when the foot is loaded, blowing over during the repose,
- discomfort while wearing high-heels,
- in more common for women;
The most common location: the plantar side of the foot and the palmar side of the hand.
Causes:
- wearing high-heeled shoes,
- bone defects / deformities of the feet (eg flat feet, high instep, long metatarsals, bone heights),
- body statics, abnormal gait,
- obesity,
- the decay of the fat pads on the sole of the foot,
- Short Achilles tendon;
Prevention:
- wearing properly selected footwear (thick, rubber sole, shock absorbing),
- use of foot relieving inserts,
- in the case of the presence of epidermal thickening, the use of special exfoliant cosmetics,
- systematic removal of poroma (pumice, pedicure)
In the podiatric office: painless removal using cutters.
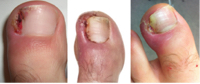 INCARNATED UNGUIS
INCARNATED UNGUIS
An ingrowing nail (Latin: Unguis incarnatus or Onychocryptosis) - a disease state in which, as a result of the pressure of the deformed nail plate, the epidermis of the surrounding tissues breaks and the lateral parts of the nail insert into the nail shaft.
Symptoms:
- soreness of the nails, redness and swelling (inflammation),
- serous exudate,
- phlegic exudation - the result of secondary infection within the wound created by irritating soft tissues through the hard plate and the presence of microorganisms,
- hypergranulation (granulation) - long-term exposure of the tissue around the nail to pressure or ingrownness;
The most common location: toes, less often toes of the foot. Young people are the most exposed to occur at the age of 14 -30 years, more often men.
Causes:
- intrinsic factors:
- bone and joint diseases, foot deformities (mainly crooked toe and rigid toe),
- abnormal shape and structure of the nail plate,
- hypertrophy of lateral nail ducts,,
- microcirculation disorders,
- obesity,
- hyperhidrosis of the feet;
External factors:
- too tight footwear exerting pressure on the forefoot,
- footwear with high heels forcing pressure on the forefoot during walking,
- inadequate shortening and giving shape to the free edge of the nail,
- mechanical injury;
Prevention:
- proper shortening of nail plates straight, without rounding the edges and without cutting them,
- proper selection of footwear (not too tight or too loose, avoiding wearing high-heeled shoes),
- regular performance of specialist pedicures;
In the podiatric office:
Swabbing consist in placing a soft and thin dressing material in the space between the fingernail and the side shaft. The most commonly used dressing materials used in tamponing include: Felteline, cotton, Ligasano® dressing. These materials can be soaked in liquids soothing inflammation, healing or disinfecting. Tamponada works well in case of exudate.
Sulci-Protector tubes - isolate the nail shaft from the nail plate. Their use brings results in the case of badly cut nails, because it prevents the change of the direction of the growing nail. Tubes are also recommended for people who can not cope with the use of tamponade, e.g. in the elderly. They can not be used in cases of exudate and with increased pain.
Taping involves the abduction of the nail shaft tissue from the nail plate. Taping is, however, not very popular and rarely used to treat this disease.
Clasps therapy (orthonyxia) - podology technique used for ingrown and screwing nails. It is a method of correction of nails by lifting the edges of the nail and changing the direction of its growth in case of ingrowth. The main characteristics of buckles include: immediate pain relief, safety of use, non-invasive. The buckles do not turn off the patient from daily activity, they do not cause pain. They are one of the most commonly used methods of correction of ingrown nails due to the possibility of individual adjustment to the existing problem, the condition of the nails and the effectiveness of the therapy.
In the absence of efficacy of conservative treatment, surgical methods are used (eg. removal of all or part of the nail, reduction of lateral nail ducts).
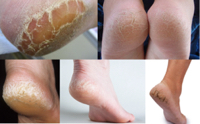 FEET KERATOSIS AND CRACKED HEELS
FEET KERATOSIS AND CRACKED HEELS
Symptoms:
- skin thickened, not very elastic with a yellowish tinge,
- often furrows and fissures, which can become a ground for inflammation,
- heel cracks often with their bleeding;
The most common location: soles of the feet, heels.
Causes:
- overweight,
- ponderous walk,
- stiff shoes,
- dry skin,
- keratinizing or other dermatological diseases,
- diabetes;
In the podiatric office: we pull the skin callus (chisel, scalpel, cutter) off, leveling the epidermis. If there is a wound, we put on dressings. With each treatment the skin on the heel becomes more delicate and the cracks are shallower, until they disappear.
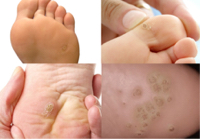 WARTS
WARTS
Foot warts (verrucae plantares) - follicular lesions located on the plantar part of the feet, have a rough, uneven surface and skin color, can reach 1-2 cm in size. They are twofold: scattered, deep (myrmecia) or more superficial, merging into clusters forming the so-called mosaic warts. Myrmecia type warts are often painful and can make it difficult to walk. The agent that causes meyrmission is HPV-1 virus, mosaic warts are caused by HPV-2. It is assumed that up to 10% of humanity is infected with papilloma virus. Children and young adults are particularly vulnerable (contact with places such as sandpits, swimming pools or gyms), as well as people with immunodeficiency diseases such as AIDS, lymphoma, immunosuppressive treatment and suffering from atopic dermatitis.
Przyjmuje się, że nawet do 10% ludzkości zarażonych jest wirusem brodawczaka. Szczególnie narażone są dzieci i młodzi dorośli (kontaktem z takimi miejscami jak piaskownice, baseny czy sale gimnastyczne), a także osoby z chorobami przebiegającymi z obniżeniem odporności, takie jak AIDS, chłoniak, leczone immunosupresyjnie i cierpiące na atopowe zapalenie skóry.
Treatment: due to the infectious character, warts are treated pharmacologically or surgically. It is possible to give up the changes spontaneously.
In the podology clinic - during the pharmacological therapy, you can remove calluses for better drug penetration (absorption).
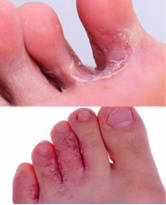 ATHLETE’S FOOT
ATHLETE’S FOOT
The term "athlete's foot" is defined as a skin infection caused by fungi, mainly by dermatophytes, on the plantar surface of the feet, toes and interdigital folds. There are three main cultivars of foot fungus: interdigital, follicular and exfoliative.
Tinea pedum interdigitale is the most common form of foot mycosis. Changes are located in the interphalanal spaces of the feet (usually III and IV space), where fungus find excellent living conditions, due to high humidity and elevated temperature. Exfoliation, maceration of the epidermis and cracks dominate the clinical setting. The erythema is visible beneath the macerated epidermis. The surface of changes is often damp, with a white-grayish color. Occasionally, the lesions spread beyond the interdigital regions, including the surfaces of the fingers. Not infrequently, tinea pedis is the source of infection of the toenails. Skin changes are often accompanied by pruritus.
Follicular mycosis (tinea pedum dyshidrotica) - this form is also called dyshydrotic. The clinical picture is dominated by focuses of grouped vesicles with serous content, on the erythematous base, most often located on the soles of the feet. The evolution of changes consists in the blistering and breakage, followed by the appearance of exfoliation.
Exfoliating exanthema mycosis (tinea pedum desquamativa) - this is a variety with an extremely chronic course. It is characterized by erythematous changes with hyperkeratosis, with a dry, as if flaky surface (fine-grained exfoliation). These changes often include entire soles and can pass to the side surfaces of the feet, and sometimes even on their backs. Because they resemble the shape of moccasin, this type of athlete's foot is also called moccasin fungus.
In the podiatry office: mycosis requires pharmacological treatment, so a visit to a dermatologist is necessary. After treatment, you can use treatments that will exfoliate and moisturize the skin of the feet.
Prophylaxis of onychomycosis:
- do not borrow shoes, do not try on other people's shoes,
- care for proper drying of the feet (hyperhidrosis promotes maceration of the epidermis and increases the risk of infection) - use deodorants, inserts, etc.,
- avoid wearing socks/tights with a large admixture of artificial fibers,
- wear airy leather shoes,
- avoid unmatched shoes which may cause abrasions and minor injuries,
- at the pool, in the gym, hotels and other public utility places, use the safety flaps and disinfect the feet after contact with the surface,
- do not use other pedicure supplies, towels, sponges, etc,;
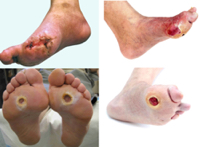 DIABETIC FOOT
DIABETIC FOOT
Diabetic Foot Syndrome (SSC) is a group of symptoms associated with long-lasting diabetes, its consequences: angio- and polyneuropathy and the risks that may occur on their background. In people with diabetes, the risk of a chronic wound on the lower extremities is 20 to 50 times higher than in healthy people. Angiopathy is responsible for hypoxia and malnutrition of tissues, including nervous tissue, which causes polyneuropathy. Diabetic polyneuropathy means that the patient does not record tissue damage, which leads to deformation and chronic changes in wounds and ulcers.
Additional factors favoring the appearance of diabetic foot:
- incorrectly selected footwear,
- obesity,
- the type of work performed,
- incorrect control of glycemic levels,
- burning tobacco,
- blood pressure problems,
- deformations of the foot,
- endured diabetic foot syndrome in the past,
- the elderly age;
Treatment: consists mainly of proper control of blood sugar levels. Difficulty of healing wounds, sores or focal points of necrosis require surgical supply. Less severe changes consisting of calluses and minor wounds are provided in podology offices.
Prevention of diabetic foot:
- Regular inspection of the feet by a family member or professional
- Noninvasive removal of hyperkeratoses
- protection against injuries and scarrings
- Frequency shortening of nails
- wearing of well-attuned footwear;
 PACHYONYCHIA
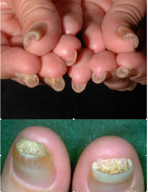
PACHYONYCHIA
The thickness of nails may increase at manual workers, in many diseases, and also during the use of certain medications. A special form of pachyonychia is the nail spontaneity - onychogryphosis, which most often affects nails of the big toe fingers of the elderly. It is usually caused by injuries, tight footwear, negligence in clipping nails, peripheral circulation disorders and dermatological diseases (including psoriasis, athlete's foot, contact dermatitis, lichen planus, alopecia areata).
In the podiatric office: cleansing from horny masses.
 SEPARATING THE NAIL BOARD (ONYCHOLIS)
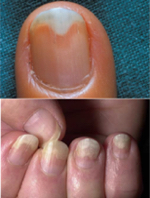
SEPARATING THE NAIL BOARD (ONYCHOLIS)
Onycholysis is the separation of the nail plate from the placenta in its distal and / or lateral part. The changes usually start at the end of one or several nails and grow until one third of the nail has separated. The separated area is pale due to the loss of light reflection from the nail bed. Onycholysis creates a subungual space in which contaminants and exfoliated keratin can accumulate, which causes a variety of nail discoloration from white through gray, yellow, brown to black, depending on the etiology of change. Pain may occur if you continue to stretch under the influence of an injury or additional active infection. Most often they are mixed infections, including C. albicans and many bacteria, of which the blue oil rod seems to be the most important. If the symptoms persist for several months, the nail bed becomes dark and irregularly thickened. We distinguish inherited and / or congenital onycholysis and acquired onycholysis: exogenous, endogenous and idiopathic.
Exogenous causes of onycholysis::
- Injuries: long-distance running, tennis, basketball and other types of sports requiring rapid change in the direction of constant movement energy may cause onycholysis with or without subungual hematomas. Changes in the biomechanics of the lower limbs, which appear with age, orthopedic changes, edema, arthritis, etc. can diversify the feet in various ways, transferring forces from the heel area to the nails of the feet. High heels and unmatched or too-tight shoes are often the reason for nail changes,
- Accidental, professional, self-injury, scratch, crush, jam,
- Contact with chemicals: accidental, professional, nail cosmetics,
- infections: fungi, bacteria, viruses (eg. warts, herpes, shingles), scabies
- moisture
- pharmaceuticals (doxycycline, 8-methoxypsoralen, retinoids)
Endogenous causes of onycholysis: :
- Skin diseases: psoriasis, lichen planus, alopecia areata, Darier's disease, bladder diseases, Reiter's syndrome, atopic dermatitis, contact dermatitis, mycosis fungoides, hyperhidrosis, multifocal reticulohistiocytosis, scleroderma
- Systemic disorders: peripheral circulation disorders, lung cancer, collagen diseases, thyroid diseases (hypofunction, hyperthyroidism), syphilis, iron deficiency, multiple myeloma, bronchiectasis, diabetes, histiocytosis X, leprosy, lupus erythematosus, pellagra, porphyria, syphilis II and III period, a band of yellow nails
- pregnancy;
In the podiatric office: delicate removal of the dead part of the separated plate, cleaning the space under the separated plate (infection prophylaxis).
 Fungoid nail’s disease
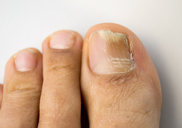
Fungoid nail’s disease
Nail fungus (Latin onychomycosis, tinea unguinum) - a disease that may be accompanied by foot and hand fungus, as well as other forms of skin mycosis. The infected nail loses its pink color, becomes crushed and crumbles easily. The epidermis under the thickened and cracked edge of the plate undergoes excessive keratosis. These changes can last a long time and make for the patient an annoying difficulty in everyday life, and for his environment a source of indirect or direct infection.
Treatment: onychomycosis requires pharmacological treatment (general and / or local), and laser therapies are now also being used.
In a podiatric office: depending on the form of treatment, it can recommend removing the excess nail, or the entire plate by the podologist and filling the cavity with antifungal mass.
 RECONSTRUCTIONS OF NAILS PLATES
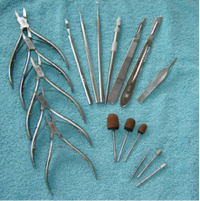
RECONSTRUCTIONS OF NAILS PLATES
Reconstruction of the feet 'nails involves the use of a special gel mass to make up the missing part of the nail. The condition for the reconstruction with gel masses is the patient's toenail in at least 1/3 of its length. In addition, the natural nail plate must be cleansed and free from ringworm. Fragile and woody nails must be accurately milled and cleaned.
Although gel masses used to reconstruct nails in addition to adhesive properties have antifungal ingredients, they are not medicinal preparations but prevent the formation of old and new states of fungal sources during reconstruction.
In the podiatric office: we create a special mass of cured nail plate (the mass has antifungal properties), which is also suitable for painting; the aim is primarily the aesthetic appearance, but also the invaluable sense of comfort of the patient and increase the sense of self-worth.
We use this treatment:
- Cosmetically - when the plate does not grow back at all after surgery or is very deformed.
- Medicinally:
- when there is a hematoma as a result of mechanical damage and there is a possibility that the new nail will grow into the nail shaft.
- for the treatment of onychomycosis, when we remove most of the horny masses of the molded nail as a protection against ingrowing into the shafts of the newly growing healthy nail.
How to avoid the need for reconstructing your nails:
- protect the toes of the feet against excessive pressure in the footwear,
- If you notice the first symptoms resembling a hematoma under the fingernail - contact the podologist as soon as possible,
- Wear protective rings with soft silicone to protect against pressure on the bearing and the missing nail,
- Do not remove the growing nails surgically if you do not use other methods, eg. orthonyx staples for ingrown nails;

