Removal of skin birthmarks
Nevi (commonly named birthmarks or beauty marks) are developmental irregularities on the skin, which are present at birth (inborn), however sometimes they develop later in life (acquired). They can appear throughout whole life. Depending on the the skin structure they are derived from, birthmarks (nevi) are classified into the following types:
Epidermal nevi
Seborrhoic warts (senile warts)
 They are included to the group of epidermal nevi, which are in fact noncancerous (benign) skin growths, characterised by warty, often hyperkeratotic surface, sometimes pedunculated (lesion attached to skin by a narrow stalk).
They are included to the group of epidermal nevi, which are in fact noncancerous (benign) skin growths, characterised by warty, often hyperkeratotic surface, sometimes pedunculated (lesion attached to skin by a narrow stalk).
The skin lesions differ morphologically: from flat raised, well marked off from the surrounding skin papules which are flesh coloured, to raised, warty, hyperkeratotic, dark brown overgrowths.
Location:
Most often, they can be found on the trunk of the body, on the face and the dorsal surface of hands. They often appear in middle-aged and older adults. Multiple seborrhoic warts on the trunk of the body may be a sign of cancer growth on patient's internal organs, while in some other cases - a symptom of a digestive track cancer or other cancers.
Treatment: CO2 laseroterapy, curettage, electroresection (electrosurgery).
Verrucous epidermal nevus
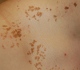 Areas of hyperpigmented plaques and/or with verrucous skin-colored papules, which tend to follow linear patterns on the skin;
Areas of hyperpigmented plaques and/or with verrucous skin-colored papules, which tend to follow linear patterns on the skin;
Treatment: CO2 laser, surgical excision;
Appendageal nevi
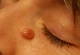 1. Nevi derived from hair fillicle
1. Nevi derived from hair fillicle
They are benign, highly structured tumors, typically occuring on the face and scalp, e.g. trichofolliculoma, trichoadenoma, trichoblastoma, trichoepithelioma, tricholemmoma, pilomatrixoma and others;
Treatment: CO2 laser/ surgical excision;
2. Nevi derived from sebaceous glands
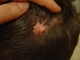 - sebaceous nevus - is a yellow or pink, verrucous lesion, hairless, present at birth (may turn darker and grow thicker with age);
- sebaceous nevus - is a yellow or pink, verrucous lesion, hairless, present at birth (may turn darker and grow thicker with age);
Location: the face and scalp (mainly: forehead, temples, cheeks, around the ears);
Treatment: surgical excision or deep ablation with CO2 laser;
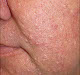 - sebaceous glands hyperplasia - single or multiple papules 1-3 mm in size, flesh-coloured or yellowish, often with a central depression, occurring mainly in middle-aged and older adults;
- sebaceous glands hyperplasia - single or multiple papules 1-3 mm in size, flesh-coloured or yellowish, often with a central depression, occurring mainly in middle-aged and older adults;
Location: face: (mainly: forehead, nose, cheek), neck;
Treatment: CO2 laser;
-other types: sebaceous cyst, sebaceous adenoma;
3. Nevi derived from sweat glands
 - syringomas - most typical appendageal nevi; small, skin-coloured or yellowish rounded bumps, typically found clustered on the eyelids of young women; although they may also be found in each area near eccrine sweat glands (trunk of the body, the labia);
- syringomas - most typical appendageal nevi; small, skin-coloured or yellowish rounded bumps, typically found clustered on the eyelids of young women; although they may also be found in each area near eccrine sweat glands (trunk of the body, the labia);
Treatment: Laser CO2 - high recurrence rate;
- other types: cylindroma, hidrocystoma (also known as cystadenoma);
Hemangiomas of the skin
Capillary hemangioma
 Hemangioma may be present already at birth, but it usually appears in 1-2 week after birth, as a tiny red bump on a child's head or other part of the body. Most intensive growth can be observed within the first 6 months of life and after 12 months it reaches its final size. It is a red, soft, raised, lumpy area, which resembles a strawberry. Most hemangiomas regress spontaneously between 5 and 9 years of age, leaving skin discolouration or a cluster of dilated capillaries.
Hemangioma may be present already at birth, but it usually appears in 1-2 week after birth, as a tiny red bump on a child's head or other part of the body. Most intensive growth can be observed within the first 6 months of life and after 12 months it reaches its final size. It is a red, soft, raised, lumpy area, which resembles a strawberry. Most hemangiomas regress spontaneously between 5 and 9 years of age, leaving skin discolouration or a cluster of dilated capillaries.
Treatment: surgical excision, laseroterapy, cryotherapy. Hemangiomas may regress spontaneously.
Pyogenic granuloma
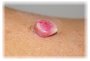 A hemangioma connected with carcinogenesis of capillaries, due to irritation, physical trauma and/or bacterial infection. It usually appears as a single, red/pink to purple nodule, with a moist, prone to bleeding surface and pedunculated base. Pyogenic granulomas can grow rapidly. They often appear during pregnancy or as a complication of oral isotretinoin therapy. Typically, they can be found on the face and hands. The lesions are painless.
A hemangioma connected with carcinogenesis of capillaries, due to irritation, physical trauma and/or bacterial infection. It usually appears as a single, red/pink to purple nodule, with a moist, prone to bleeding surface and pedunculated base. Pyogenic granulomas can grow rapidly. They often appear during pregnancy or as a complication of oral isotretinoin therapy. Typically, they can be found on the face and hands. The lesions are painless.
Treatment: Lasotherapy with CO2 laser, surgical removal, electrocoagulation; frequent recurrence.
Venous lake
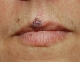 A vascular lesion: soft, compressible, dark blue papules, occurring mainly on the vermilion border of the lip or on the ear lobe.
A vascular lesion: soft, compressible, dark blue papules, occurring mainly on the vermilion border of the lip or on the ear lobe.
Treatment: CO2 laser or surgical excision;
Melanocytic nevi
Melanocytic nevi (the name comes from melanocyte - a cell producing the skin pigment - melanin) are inborn skin irregularities, which many times appear in elder patients.
1. Epidermal melanocytic nevi
- flat nevi - not raised from the level of the skin, with a clearly-defined edge, do not cause any discomfort. They expand as the child grows. In case of frequent irritation of the lesions they might turn into malignant skin cancer - melanoma, however it happens very rarely.
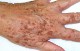 - lentigines - small, pigmented, light or dark brown spots on the skin with clearly-defined edges. They usually occur as multiple lesions. Typically, they can be found on the trunk of the body and they develop in childhood. They resemble freckles, but are slightly larger. Solar lentigines or old age spots are associated with exposure to ultraviolet radiation from the sun or caused by PUVA therapy. They also occur on the skin of ageing people or people with fair complexion (difficult to tan). In fact, they are just a cosmetic defect. The lesions may be single or multiple, located in areas most often exposed
to the sun, particularly the hands, face, shoulders, arms and forehead. They appear more numerously in the summer and also they darken at this time of a year. Solar lentigines may gradually and spontaneously fade, while the old age spots are permanent. So called lentigo maligna may turn into lentigo maligna melanoma. The lesions are then dark with irregular pigmentation with a bumpy surface. They may be found on the face, more often in women and elderly people. In such cases, the evolution to lentigo maligna melanoma is very slow and the course of disease is relatively mild.
- lentigines - small, pigmented, light or dark brown spots on the skin with clearly-defined edges. They usually occur as multiple lesions. Typically, they can be found on the trunk of the body and they develop in childhood. They resemble freckles, but are slightly larger. Solar lentigines or old age spots are associated with exposure to ultraviolet radiation from the sun or caused by PUVA therapy. They also occur on the skin of ageing people or people with fair complexion (difficult to tan). In fact, they are just a cosmetic defect. The lesions may be single or multiple, located in areas most often exposed
to the sun, particularly the hands, face, shoulders, arms and forehead. They appear more numerously in the summer and also they darken at this time of a year. Solar lentigines may gradually and spontaneously fade, while the old age spots are permanent. So called lentigo maligna may turn into lentigo maligna melanoma. The lesions are then dark with irregular pigmentation with a bumpy surface. They may be found on the face, more often in women and elderly people. In such cases, the evolution to lentigo maligna melanoma is very slow and the course of disease is relatively mild.
2. Cellular melanocytic nevi
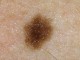 These are very frequent nevi, may be of a skin-like colour, but they range from light to a very dark brown. Their surface varies from smooth, through verrucous to lobular. They may be flat, raised, nodular or even pedunculated or hairy. Practically, more than ten such lesions can be found on the skin of every human. The risk of their malignant transformation is low. Higher risk is associated with the lesions which are raised, pedunculated and hairy, the most dangerous are the inborn and dysplastic nevi. The number of acquired melanocytic nevi in people of white human race is usually high - there might be dozen
or so lesions of this type. They often appear in early childhood, however, we acquire most of them at the age of 20-30. The risk of the melanoma development is low, especially in the raised, pedunculated and hairy lesions, though it is probable in the case of inborn and dysplastic nevi. The possible symptoms of melanoma development include:
These are very frequent nevi, may be of a skin-like colour, but they range from light to a very dark brown. Their surface varies from smooth, through verrucous to lobular. They may be flat, raised, nodular or even pedunculated or hairy. Practically, more than ten such lesions can be found on the skin of every human. The risk of their malignant transformation is low. Higher risk is associated with the lesions which are raised, pedunculated and hairy, the most dangerous are the inborn and dysplastic nevi. The number of acquired melanocytic nevi in people of white human race is usually high - there might be dozen
or so lesions of this type. They often appear in early childhood, however, we acquire most of them at the age of 20-30. The risk of the melanoma development is low, especially in the raised, pedunculated and hairy lesions, though it is probable in the case of inborn and dysplastic nevi. The possible symptoms of melanoma development include:
- elevation, such as thickening or raising of a previously flat lesion
- the pigmentation is not uniform: shades of brown and black are present, changes in colour distribution, especially the spread of colour from the edge of a mole into the surrounding skin
- sensation, such as itching, tingling, or burning
- scaling, erosion, oozing, bleeding, or crusting of the surface
Dark stripes or bands seen through the nails of the thumb, forefinger, or great toe can indicate the presence of melanoma, which, considering the diagnostic problems and differentiation from melanoma, should be always surgically removed.
 - Inborn melanocytic nevi are usually large - they typically have many centimetres, sometimes they have uneven, verrucous sufrace with fine hairs. Although these features are considered "safe" (bengin), the risk of melanoma development is higher than in the group of acquired nevi. Sometimes the nevi cover large areas of the body, e.g. whole trunk of the body.
- Inborn melanocytic nevi are usually large - they typically have many centimetres, sometimes they have uneven, verrucous sufrace with fine hairs. Although these features are considered "safe" (bengin), the risk of melanoma development is higher than in the group of acquired nevi. Sometimes the nevi cover large areas of the body, e.g. whole trunk of the body.
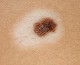 - Sutton nevus (halo nevus) - is a mole that is surrounded by a depigmented ring, typically undergoes regression; can be found mainly in children and appear when white blood cells target a mole; is more prevalent in people with vitiligo; considered as harmless (no risk of cancer).
- Sutton nevus (halo nevus) - is a mole that is surrounded by a depigmented ring, typically undergoes regression; can be found mainly in children and appear when white blood cells target a mole; is more prevalent in people with vitiligo; considered as harmless (no risk of cancer).
Treatment: only of cosmetic significance, no treatment is required, eventual surgical excision;
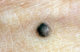 - Blue nevus - its melanocytes are quite deep in the skin, can be found on the face and limbs. Their colouring ranges from light-blue to black. They belong to so called safe (non-cancerous) nevi, meaning only rarely they may transform into melanoma.
- Blue nevus - its melanocytes are quite deep in the skin, can be found on the face and limbs. Their colouring ranges from light-blue to black. They belong to so called safe (non-cancerous) nevi, meaning only rarely they may transform into melanoma.
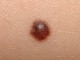 - Spits nevus - until recently, it has been known under its misleading term of a juvenile melanoma. It is not a melanoma, it is a benign lesion and the term derived from its similarities to melanoma in histologic image. They are most often found in young people on the face, less often on the limbs. The nevi are usually single, red or bluish, sometimes the main lesion is surrounded by smaller lesions - satellite nevi.
- Spits nevus - until recently, it has been known under its misleading term of a juvenile melanoma. It is not a melanoma, it is a benign lesion and the term derived from its similarities to melanoma in histologic image. They are most often found in young people on the face, less often on the limbs. The nevi are usually single, red or bluish, sometimes the main lesion is surrounded by smaller lesions - satellite nevi.
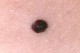 - Reed nevus - rapidly growing lesion (which may suggest melanoma), of uniform dark-brown colour, flat or raised, with diameter up to 1 cm, mainly occurring on the limbs; treatment: surgical excision.
- Reed nevus - rapidly growing lesion (which may suggest melanoma), of uniform dark-brown colour, flat or raised, with diameter up to 1 cm, mainly occurring on the limbs; treatment: surgical excision.
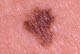 - Dysplastic nevus is reported in 5-8% of white race human, and the so called dysplastic nevus syndrome is often a hereditary condition. They can be found all over the body, including the scalp, where they might become especially dangerous, considering constant iritation and limited observation.
- Dysplastic nevus is reported in 5-8% of white race human, and the so called dysplastic nevus syndrome is often a hereditary condition. They can be found all over the body, including the scalp, where they might become especially dangerous, considering constant iritation and limited observation.
 - Dysplastic nevus syndrome is often a hereditary condition. The syndrome carries a great risk of undergoing malignant transformation and therefore plays a signifficant role, considering the measures for prevention of melanoma. Dysplastic nevi have the following features:
- Dysplastic nevus syndrome is often a hereditary condition. The syndrome carries a great risk of undergoing malignant transformation and therefore plays a signifficant role, considering the measures for prevention of melanoma. Dysplastic nevi have the following features:
- they occur in a few or many family members
- they are usually numerous
- they are bigger in size than other nevi (5-15 mm)
- they have irregular borders and multiple colours
- they are either flat or unevenly raised in the central part of the nevi, or with irregular surface
Dysplastic nevi are most numerous at the age from 6 months to 30 years, but also later in life, but then they are less plentiful. In a number of patients they regress spontaneously. Dysplastic nevi are more likely to undergo malignant transformation, therefore, they require regular medical examinations (every 3-12 months) and efficient sun protection.
Removal of melanocytic nevi
Early surgical removal of malignant nevi saves lives in very many cases. However, one must be very careful deciding about removal of nevi. Evaluation of melanocytic nevi is incredibly difficult, even with such professional device as dermatoscope. Therefore, the experience and competence of medical staff plays major role here. Majority of lesions are removed mainly because of cosmetic concern. If the lesion is suspected to be a skin cancer, the safest method of its removal is surgical treatment and histopathological examination of the removed lesion.
Such lesions should never be sampled for examination, considering the risk of their malignant transformation as an effect of irritation.
If a dysplastic nevus is suspected of being a melanoma, it should be surgically removed with
some margin of healthy skin.
REMEMBER !!!
- Before starting any treatment of birthmarks and pigmented lesions, you should always consult a dermatologist.
- If you notice any change in your melanocytic naevi, you should see your doctor immediately. Postponing the consultation may only worsen the situation.
- Any suspicion of malignant transformation is an unconditional indication for surgical treatment.
- The melanocytic nevi should not be removed with laser, as the performance of histopathological examination is then impossible. In order to remove a birthmark with the laser method, the doctor must be one hundred percent sure that the lesion is not malignant.

